Springer Link-Journal Article – Breast Lift Surgery
Background
Numerous techniques have been described for the treatment of breast hypertrophy and ptosis. Unfortunately, recurrent ptosis after mammaplasty can occur regardless of the technique used. To avoid this problem, different kinds of supporting devices have been described with variable rates of success. However, the true implications of incorporating prosthetic materials into breast surgery have never been clarified. Therefore, surgeons have traditionally been reluctant to apply any kind of prosthetic material to the breast, fearing inflammation, an unfavorable aesthetic outcome, palpable or visible deformities, and interference with the mammographic evaluation of breast cancer. This study analyzed the aesthetic, clinical, and mammographic implications of using mesh as a supportive device in periareolar breast surgery.
Methods
For this study, 18 patients (mean age, 42 years) with breast hypertrophy, ptosis, or both were managed with the double-skin periareolar mammaplasty technique, with placement of mixed (60% Polyglactine and 40% polyester) mesh. Clinical assessment was performed by three breast surgeons actively working on cancer surveillance who knew that the patients had experienced mesh application. After a mean follow-up period of 30 months, a standard mammogram was performed for each patient and analyzed by both the surgeons and an expert radiologist. The evaluated factors were hyperemia, calcifications, contour irregularities, capsular contraction, thickening or widening of the scar with extrusion of the mesh, and any palpable or hardened areas.
Results
According to the authorsrsquo clinical observations, there were no mesh-related abnormalities in the breast; the mesh was not palpable after the operation; and there was no recurrent ptosis. In terms of mammographic imaging, the mesh was visible as a very fine line in the periphery of the breastrsquos parenchyma (measuring 0.2 mm on the lateral views) in three patients (17%). The mesh did not interfere with the visualization and analysis of the breastrsquos parenchyma. In seven patients (39%), benign localized microcalcifications were detected in the breast and no further investigation was performed. In two patients (11%), grouped calcifications were detected and biopsied, with histopathologic analysis demonstrating epithelial hyperplasia with atypia. In two patients (11%), nodules smaller than 1 cm were detected and biopsied, with histopathologic analysis demonstrating a fibroadenoma in one patient and an invasive ductal carcinoma in the other.
Conclusions
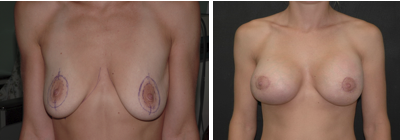
The use of mesh support in breast surgery can enhance the aesthetic results without inducing visible or palpable deformities or mammographic abnormalities. In terms of surveillance mammograms, the presence of the mesh did not interfere with the diagnosis and treatment of minute lesions such as calcifications and small nodules
The Application of Mesh Support in Periareolar Breast Surgery: Clinical and Mammographic Evaluation
João Carlos Sampaio Góes , Alan Landecker, Eduardo Carneiro Lyra, Leonardo José Henríquez, Renata Sampaio Góes1 and Paulo M. Godoy1
For more information visit Springer Link
 (561) 394-6656
(561) 394-6656